
Best adjuvant (assist) for chemotherapy | 1+1>487% |
Effectively improve chemotherapy effect, treatment, immunity.
Reduce side effects and recurrence.
Overview / Relation / Abstract / Role / Principle / Action / Mechanism / Function / Work |
Ovarian, Fallopian Tube, and Peritoneal Cancer: Latest Research
Abstract / Summary / Overview of Apoptosis.
Why do cells undergo apoptosis?
The relationship between cancer cells and apoptosis.
Where are the weaknesses and symptoms of cancer cells?
Are cancer cells aggressive?
Extraordinary Solamargine (Role, Principle, Action, Mechanism, Function, Work)
Solamargine's major function mechanism:
Solamargine vs cancer
Best Chemotherapy Adjuvant. (1+1>478%)
Effectively improve chemotherapy effect and cure.
When cancer cells are less resistant to drugs, chemotherapy becomes more effective.
Extract : https://www.cancer.net/cancer-types/
Ovarian, Fallopian Tube, and Peritoneal Cancer: Latest Research
You will read about the scientific research being done to learn more about this type of cancer and how to treat it.
Doctors are working to learn more about ovarian/fallopian tube cancer. They are looking for ways to prevent these cancers, as well as looking for the best ways to treat them and provide care to people diagnosed with these diseases. The following areas of research may include new options for patients through clinical trials. Most ovarian cancer trials now include patients with fallopian tube and peritoneal cancers. Always talk with your doctor about the best diagnostic and treatment options for you.
Screening. In general, cancer screening is used to look for cancer before a person has any signs or symptoms. There are currently no effective screening methods for these gynecologic diseases suitable for people in the general population who are not having symptoms. A screening method study that uses serial CA-125 blood tests and pelvic ultrasonography for finding early-stage ovarian/fallopian tube cancer has been completed, and it showed no survival benefit for screening. As noted in Diagnosis and Types of Treatment, CA-125 is a substance called a tumor marker that is found in higher levels in people with ovarian/fallopian tube cancer and in people with many benign conditions.
The U.S. Preventive Services Task Force has issued a statement that says that, for the general population of people with no symptoms, screening for ovarian/fallopian tube/peritoneal cancer is not helpful and may lead to harm. This is because it can lead to an increase in unnecessary surgical operations due to "false positive" test findings.Some have recommended that people at high risk of developing ovarian/fallopian tube/peritoneal cancer because of their family history or presence of BRCA1 or BRCA2 or other high-risk gene mutation(s) (see Risk Factors) should be screened with CA-125 blood tests and transvaginal ultrasound. As stated above, this approach has not been shown to help people live longer or find cancers at an earlier and more curable stage. Therefore, if a high-risk gene mutation exists, the recommendation is to remove both fallopian tubes and ovaries after an individual finishes giving birth to children or at approximately age 40. Or, if possible, they should be removed 10 years before the age of when the individual's closest relative developed ovarian cancer.
Other targeted therapies. As described in Types of Treatment, clinical trials are ongoing for many treatments that target different mutations, including KRAS, BRAF, PI3KCA, and PTEN. Many other new, targeted treatments are now being studied in clinical trials. Increasingly, doctors are learning about each patient’s individual tumor's biology through biomarker testing. This information may be useful in matching patients with a clinical trial for a specific targeted therapy. Learn more about the basics of targeted therapy.
Immunotherapy. Immunotherapy is a systemic therapy using medication designed to boost the body’s natural defenses to fight a cancer. It uses materials made either by the body or in a laboratory to bolster, target, or restore immune system function. Researchers are examining whether drugs called checkpoint inhibitors may boost the immune system's ability to destroy cancer cells. Drugs in this category target PD-1, PD-L1, and CTLA4. They have been shown to shrink tumors in other types of cancer, such as melanoma and some lung cancers, and have had some effectiveness in certain settings for ovarian/fallopian tube cancer. Although initial trials have shown no benefit in slowing the cancer's growth, survival data is still forthcoming.
Cancer vaccines are another type of immunotherapy researchers are testing to use for ovarian/fallopian tube cancer. Some approaches, called “adoptive cell therapy,” use cells called killer T cells from the immune system in an individual patient. Researchers take these cells and grow them in the laboratory, training them to attack certain targets, such as MUC 16 (CA-125), that are found on ovarian/fallopian tube cancer cells. Doctors then put the T cells back into the patient through an IV. This approach, also called chimeric antigen receptor (CAR) T-cell therapy, has been used with some success in people with some blood cancers. Clinical trials are opening for ovarian/fallopian tube cancer. Talk with your doctor to learn more. Learn more about the basics of immunotherapy and cancer vaccines.
Hormone therapy. For treatment of recurrent or later-stage ovarian/fallopian tube cancer, tamoxifen, aromatase inhibitors, and enzalutamide (Xtandi), a blocker of the androgen receptor, as well as combining aromatase inhibitors with a CDK4/6 inhibitor such as palbociclib (Ibrance), are being studied. Learn more about hormone therapy.
Gene therapy. A new area of research is discovering how damaged genes in ovarian/fallopian tube cancer cells can be corrected or replaced. Researchers are studying the use of specially designed viruses that carry normal genes into the core of cancer cells and then replace the defective genes with functional ones.
Palliative and supportive care. Clinical trials are underway to find better ways of reducing symptoms and side effects of standard cancer treatments to improve comfort and quality of life for patients.
Abstract / Summary / Overview of Apoptosis.
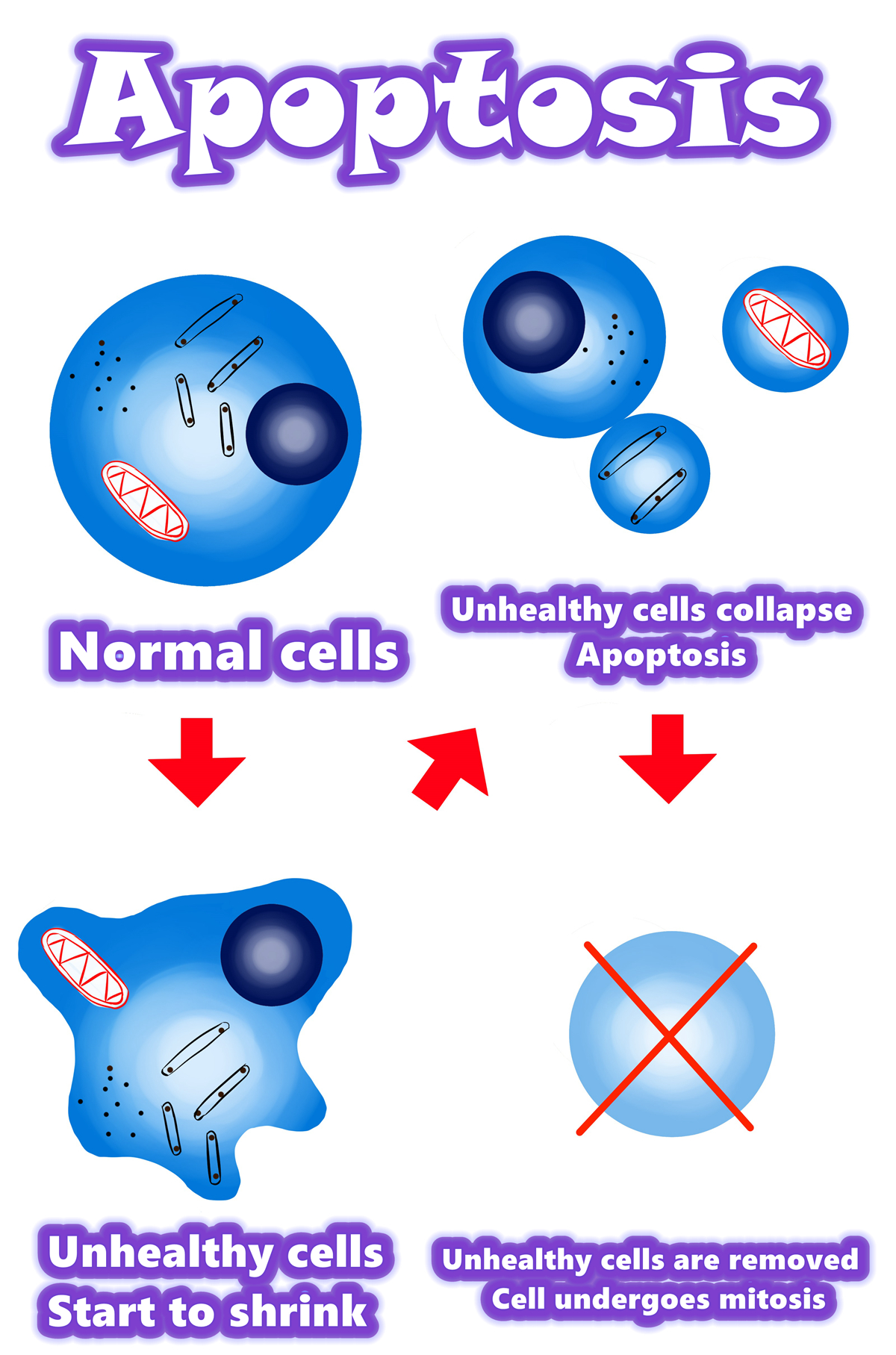
Overview of apoptosis
•Programmed cell death
•Apoptosis is a form of programmed cell death, or “cellular suicide.”
•Apoptosis is different from necrosis, in which cells die due to injury.
•Apoptosis removes cells during development, eliminates potentially cancerous and virus-infected cells, and maintains balance in the body.
Why do cells undergo apoptosis?
- Basically, apoptosis is a general and convenient way to remove cells that should no longer be part of the organism.
- Some cells are abnormal and could hurt the rest of the organism if they survive, such as cells with viral infections or DNA damage.
- Apoptosis is part of development
- In many organisms, programmed cell death is a normal part of development.
The relationship between cancer cells and apoptosis
Apoptosis can eliminate infected or cancerous cells.
When a cell’s DNA is damaged, it will typically detect the damage and try to repair it.
If the damage is beyond repair, the cell will normally send itself into apoptosis, ensuring that it will not pass on its damaged DNA.
When cells have DNA damage but fail to undergo apoptosis, they may be on the road to cancer.
However, “successful” cancer cells successfully evade the process of apoptosis.
This allows them to divide out of control and accumulate mutations (changes in their DNA).
Apoptosis is key to immune function
Apoptosis also plays an essential role in the development and maintenance of a healthy immune system.
Where are the weaknesses and symptoms of cancer cells?
The symptoms of cancer cells are in the nucleus.
The nucleus controls the outer cytoplasm, cell composition, cell viability, etc.
DNA mutations also mutate in the nucleus.
Therefore, to treat cancer cells, we must first enter the nucleus.
Let the “regulatory cell gene” mechanism enter the nucleus to regulate
Are cancer cells aggressive?
After the action of Solamargine, the aggressiveness of cancer cells is alleviated.
So after using Solamargine, many patients feel that I am half better.
Although the tumor does not disappear quickly, patients feel that the degree of aggressiveness is reduced.
Extraordinary Solamargine (Role, Principle, Action, Mechanism, Function, Work).
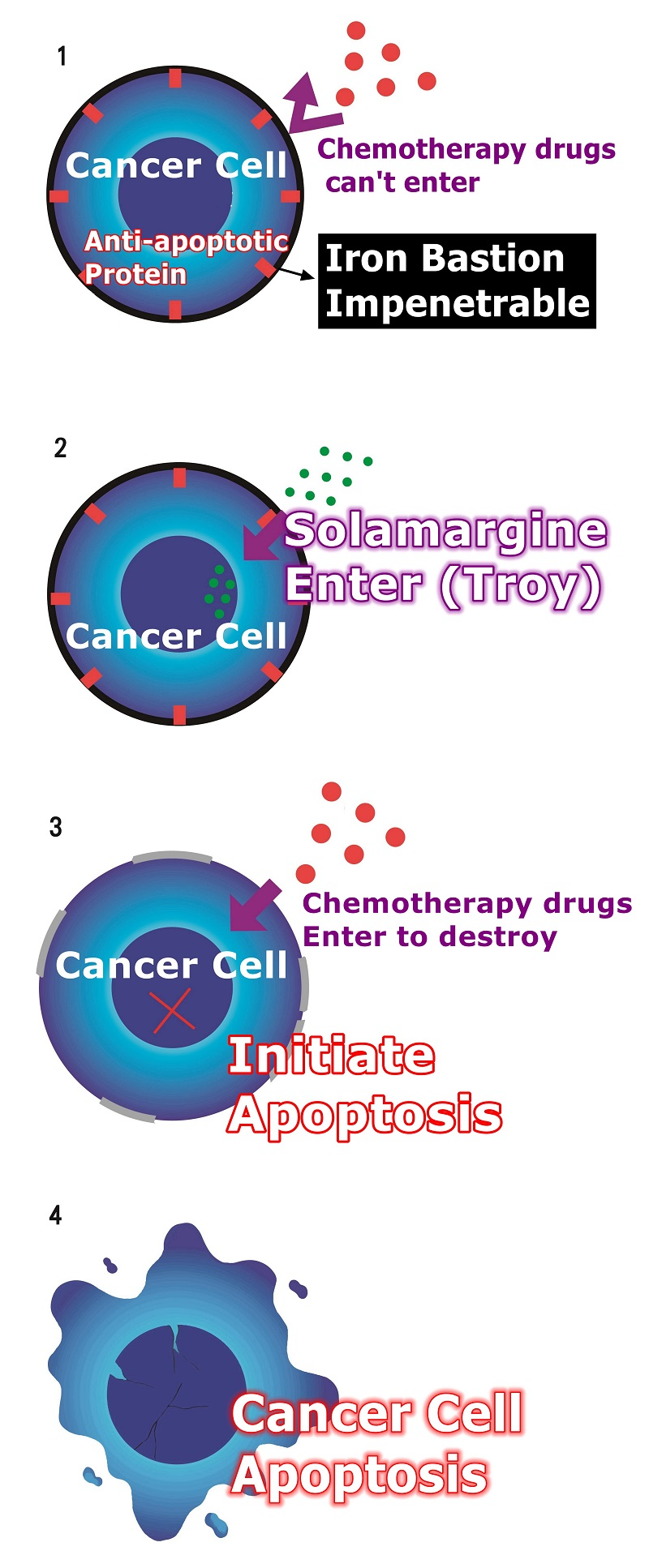
Solamargine's major function mechanism:
When Solamargine enter,
Solamargine activates receptors that are turned off by cancer cells, allowing cancer cells to modulate again.
Solamargine modulates the anti-modulates genes of cancer cells, making cancer cells less resistant.
Reduced drug resistance
When cancer cells are less resistant to drugs, chemotherapy becomes more effective.
Solamargine modulates the mutated genes in cancer cells and then initiates cancer cell apoptosis to achieve anti-cancer effects.
Solamargine combined with which chemotherapy drugs are more effective in treating cancer cells?
Solamargine vs cancer
Solamargine vs cancer
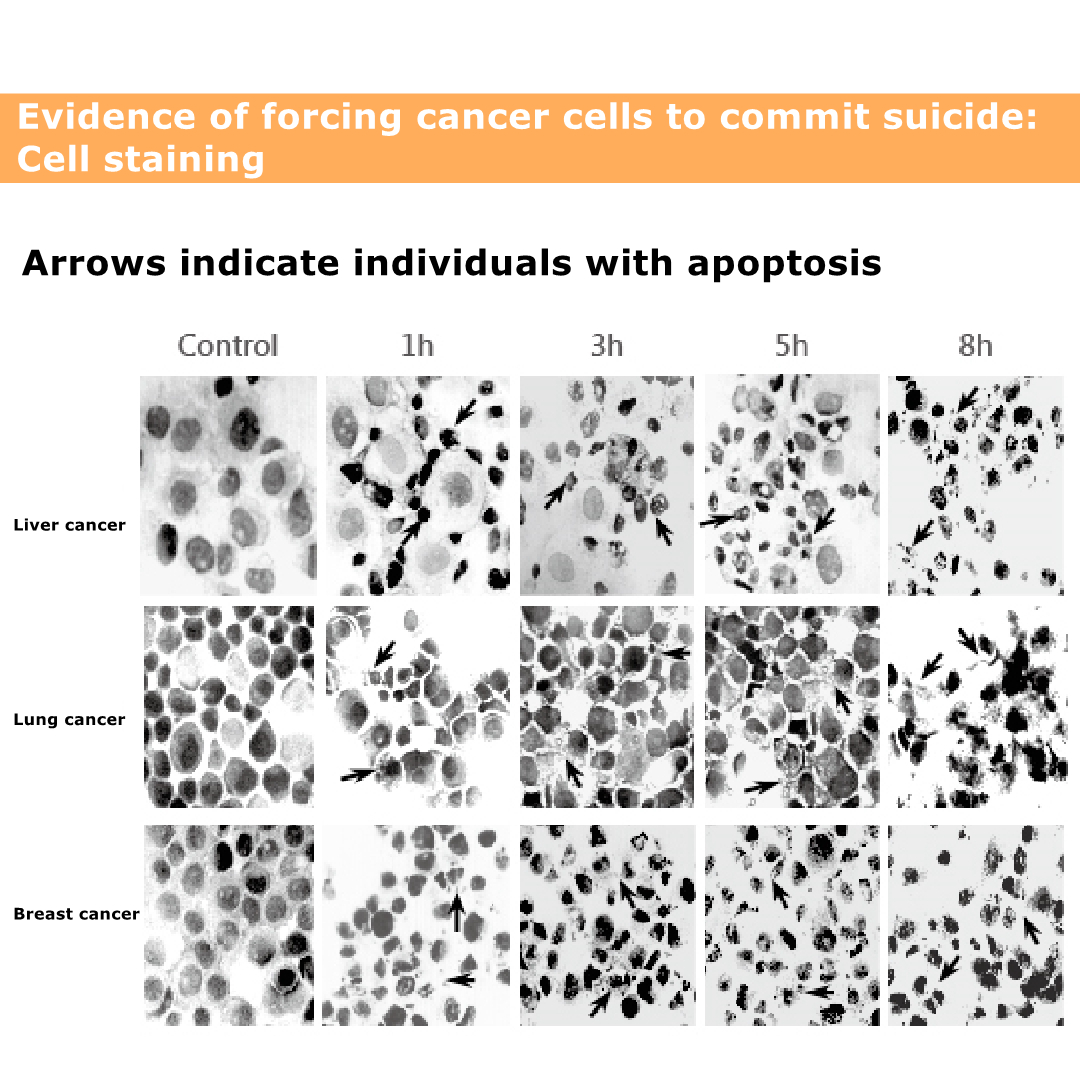
The picture shows the death of cancer cells.
The black and black parts are cancer cell nuclei.
Even if the nucleus ruptures, the cancer cells will die.
The figure shows that cancer cells can cause death.
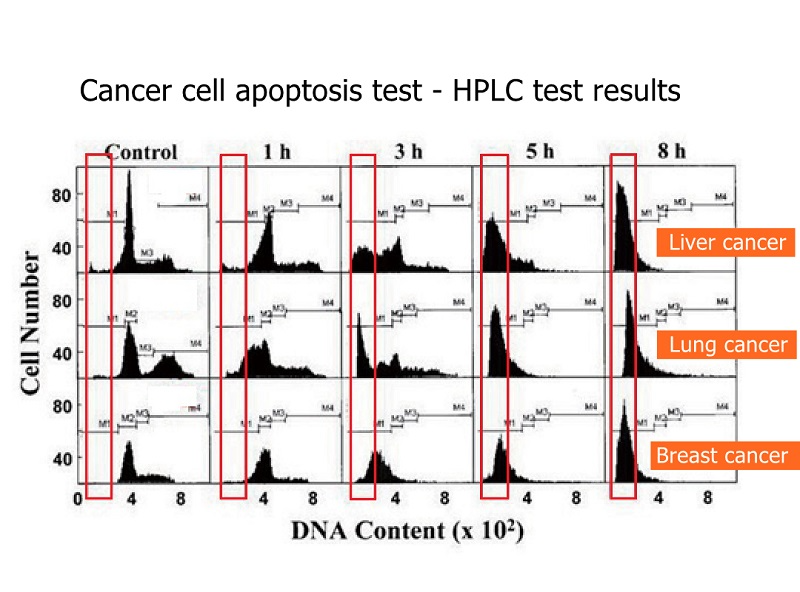
The figure shows that cancer cells can cause death.
The figure shows that the death of lung cancer cells is relatively slow, and it will not be obvious until eight hours later.
The figure shows that the death of liver cancer cells is very obvious, even more obvious in eight hours.
The graph shows that breast cancer cells die faster. It was obvious from the beginning that breast cancer is easy to treat, and patients with breast cancer need not worry.
Best Chemotherapy Adjuvant. (1+1>487%)
Effectively improve chemotherapy effect and treatment.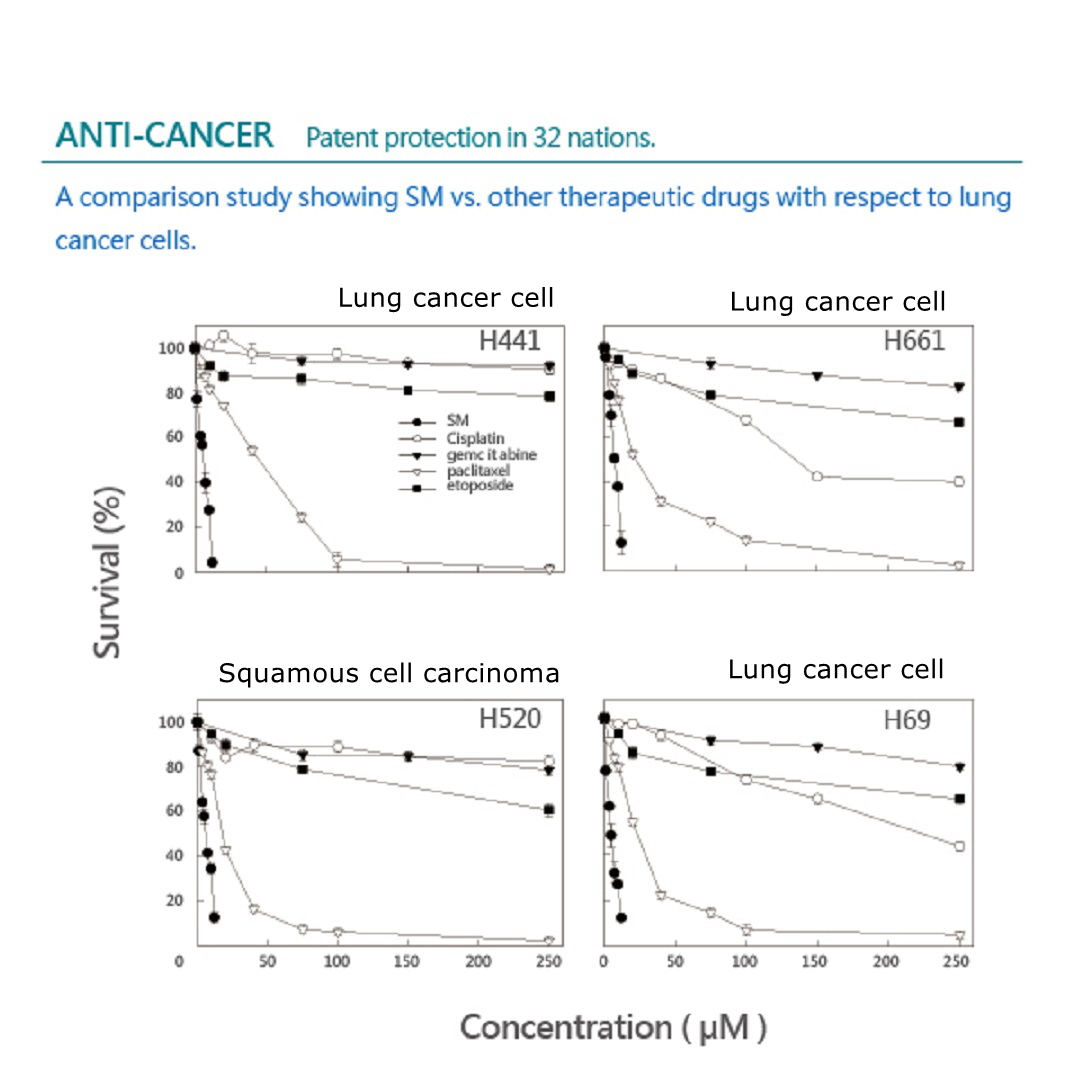
ANTI-CANCER
Patent protection in 32 nations.
A comparison study showing Solamargine vs. other therapeutic drugs with respect to lung cancer cells.
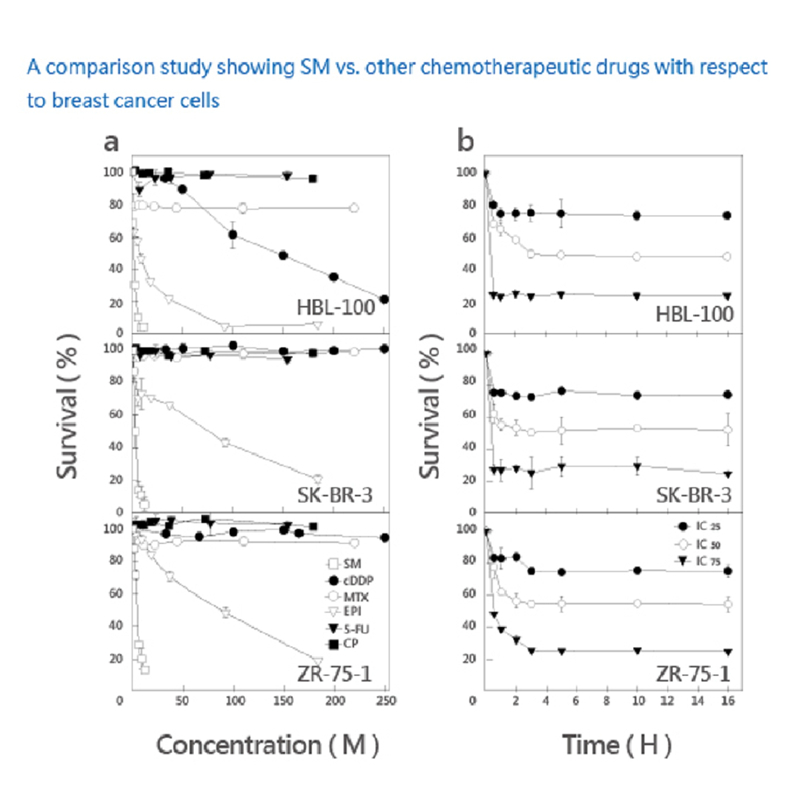 A comparison study showing Solamargine vs. other chemotherapeutic drugs with respect to breast cancer cells.
A comparison study showing Solamargine vs. other chemotherapeutic drugs with respect to breast cancer cells.
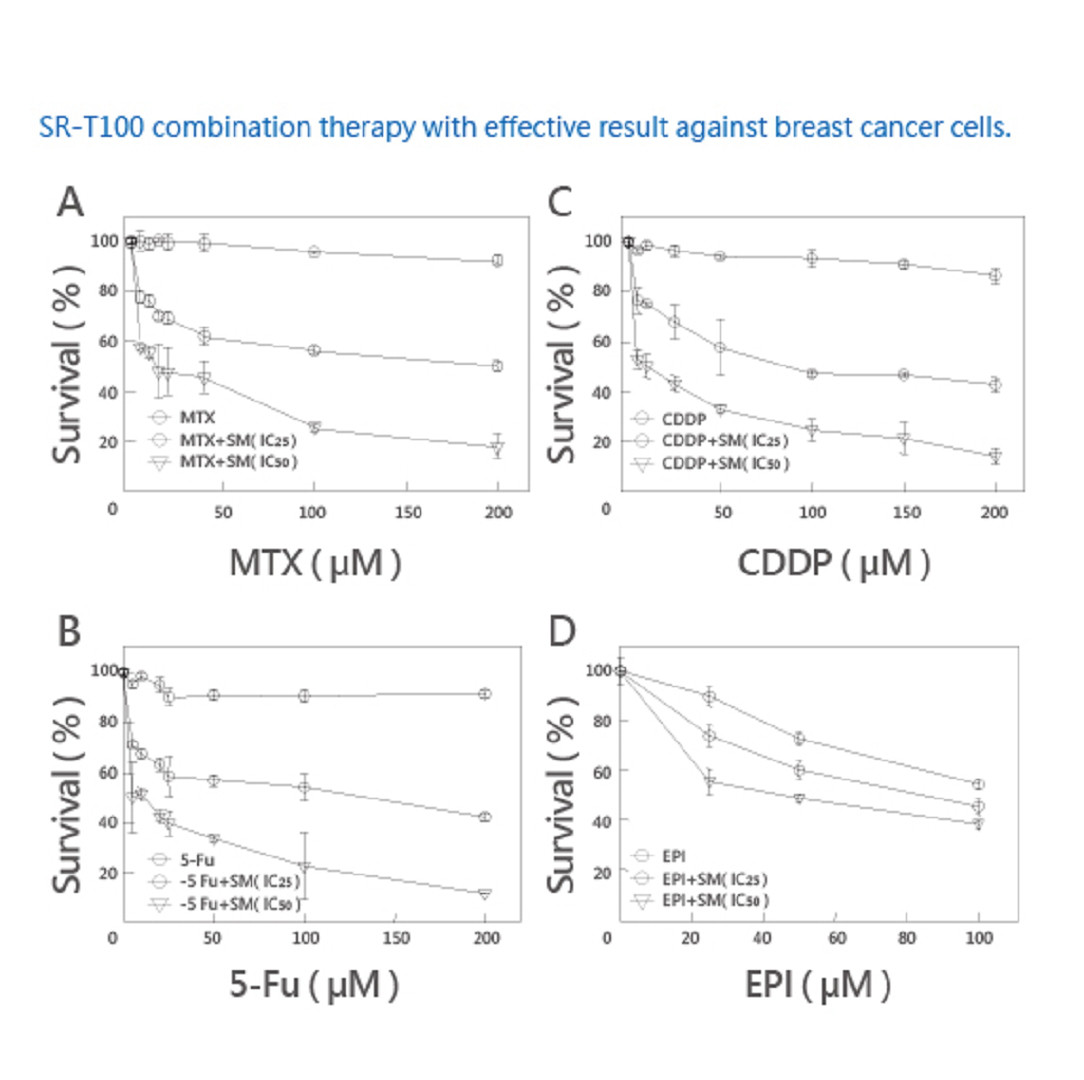
SR-T100 combination therapy with effective result against breast cancer cells.
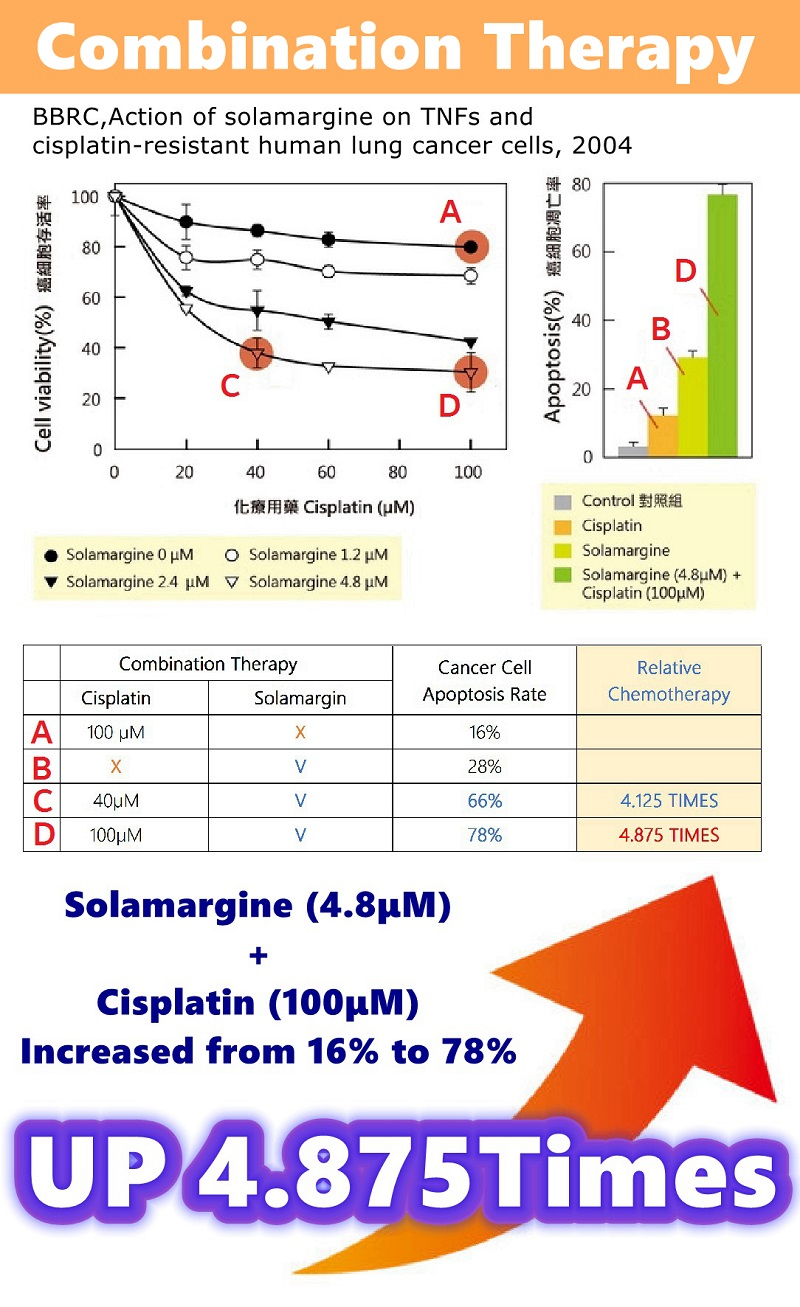
Combination Therapy | Research results for lung cancer cells.
A. Chemotherapy (100μM), 16% of cancer cell apoptosis.
B. Alone SM (4.8μM), 28% of cancer cell apoptosis.
C. SM (4.80μM) + Chemotherapy (40μM), 66% of cancer cells apoptosis.
D. SM (4.80μM) + Chemotherapy (100μM), 78% of cancer cell apoptosis.
SM has a clearing effect better than Chemotherapy.
The combined treatment of Solamargine and Chemotherapy significantly increased the apoptosis of lung cancer cells.
SM (4.8μM) + Chemotherapy (40μM), increased from 16% to 66% (up to 4.125 times).
SM (4.8μM) + Chemotherapy (100μM), increased from 16% to 78% (up to 4.875 times).
Reorganized from: BBRC. Action of Solamargine on TNFs and drug-resistant human lung cancer cells 2004.
The best solution for cancer cells.
