
Best adjuvant (assist) for chemotherapy | 1+1>487% |
Effectively improve chemotherapy effect, treatment, immunity.
Reduce side effects and recurrence.
Overview / Relation / Abstract / Role / Principle / Action / Mechanism / Function / Work |
Multiple Myeloma: Latest Research
Abstract / Summary / Overview of Apoptosis.
Why do cells undergo apoptosis?
The relationship between cancer cells and apoptosis.
Where are the weaknesses and symptoms of cancer cells?
Are cancer cells aggressive?
Extraordinary Solamargine (Role, Principle, Action, Mechanism, Function, Work)
Solamargine's major function mechanism:
Solamargine vs cancer
Best Chemotherapy Adjuvant. (1+1>478%)
Effectively improve chemotherapy effect and cure.
When cancer cells are less resistant to drugs, chemotherapy becomes more effective.
Extract : https://www.cancer.net/cancer-types/
Multiple Myeloma: Latest Research
You will read about the scientific research being done to learn more about multiple myeloma and how to treat it.
Doctors are working to learn more about myeloma, ways to prevent it, how to best treat it, and how to provide the best care to people diagnosed with this disease. The following areas of research may include new options for patients through clinical trials. Always talk with your doctor about the best diagnostic and treatment options for you. Below are some of the areas researchers are looking into. With the fast pace of myeloma research, you are encouraged to ask about available clinical trials.
New drugs. Myeloma represents a new treatment paradigm (a set of assumptions and practices) in cancer because the new drugs that target the tumor cell, tumor-bone marrow interaction, and bone marrow environment can overcome normal drug resistance. Drugs are first tested in clinical trials for advanced myeloma and then used to treat earlier-stage myeloma. A variety of new drugs are being studied for the treatment of relapsed myeloma and relapsed, refractory myeloma, including the examples below.
B-cell maturation antigen (BCMA). BCMA is a marker on the plasma cells that can be targeted for the treatment of myeloma. Several treatments that target BCMA are under development. These include antibodies that bring cells of the immune system to destroy myeloma cells, antibody-drug conjugates, and chimeric antigen receptor (CAR) T-cell therapies. Antibody-drug conjugates have shown promising early results.
Venetoclax (Venclexta, Venclyxto). This BCL-2 inhibitor has been used to treat some types of lymphoma and leukemia, and there may be benefit to using it for myeloma with a specific genetic mutation that appears in about 20% of patients with myeloma.
MCL-1 inhibitors. This class of drug destroys cells in myeloma. These inhibitors are under active development.
- Bispecific T-cell engagers (updated 10/2022). As described in Types of Treatment, bispecific antibodies are monoclonal antibodies that target a protein on the myeloma cell surface and a T cell. Clinical trials are studying this treatment in multiple myeloma, and the first bispecific T-cell engager that targets both BCMA (a myeloma marker) and CD3 (a T-cell marker) was approved to treat multiple myeloma in 2022.
Drug combinations.Most myeloma cells will eventually become resistant to standard chemotherapy, a condition called multidrug resistance. Many new drug combinations have been developed and are being studied in various settings, including:
Bortezomib and lenalidomide in combination with dexamethasone
Bortezomib, cyclophosphamide, and dexamethasone
Carfilzomib, lenalidomide, and dexamethasone
Ixazomib, lenalidomide, and dexamethasone
Pomalidomide, bortezomib, and dexamethasone
Carfilzomib, pomalidomide, and dexamethasone
Pomalidomide, ixazomib, and dexamethasone
Pomalidomide, dexamethasone, and clarithromycin (Biaxin)
Daratumumab, bortezomib, dexamethasone
Immunotherapy. This type of therapy is designed to boost the body’s natural defenses to fight cancer. It uses materials made either by the body or in a laboratory to improve, target, or restore immune system function. Vaccines are a type of immunotherapy being explored in the treatment of multiple myeloma. Research on using these therapies to treat advanced myeloma is ongoing. Learn more about the basics of immunotherapy.
CAR T-cell immunotherapy. In this type of immunotherapy, the patient’s own immune cells are removed, modified to target their own myeloma cells, and then put back into the body to fight the myeloma. One CAR T-cell therapy, idecabtagene vicleucel, has received FDA approval (see Types of Treatment), and more clinical trials are studying other CAR T-cell therapies in myeloma. Researchers are also examining the effectiveness of BCMA-targeted CAR T cells in combination with other treatments, as well as working to identify other antigens found on myeloma cells that may be effective immunotherapy targets. Learn more about how CAR T-cell therapy works to treat cancer.
Immune checkpoint inhibitors. Checkpoint inhibitor therapies include antibodies to block PD-L1 on multiple myeloma cells and PD-1 on immune cells. PD-1 is found on the surface of T cells, which are a type of white blood cell that directly helps body’s immune system fight disease. Because PD-1 keeps the immune system from destroying cancer cells, blocking PD-1 allows the immune system to better eliminate the disease. Current research is trying to work out which patients benefit most from these treatments and in which combinations of other drugs they should be used. The FDA stopped all clinical trials using PD-1 checkpoint inhibitors in multiple myeloma. In 1 study of combination therapy that included pembrolizumab (Keytruda), researchers saw an increased death rate. Other checkpoint inhibitors targeting LAG3, TIM3, and TIGIT are being studied.
Cancer vaccines. Vaccines are another type of immunotherapy being explored in the treatment of multiple myeloma. Learn more about therapeutic cancer vaccines.
Palliative care/supportive care. A limited number of clinical trials are underway to find better ways of reducing symptoms and side effects of current myeloma treatments to improve comfort and quality of life for patients.
Abstract / Summary / Overview of Apoptosis.
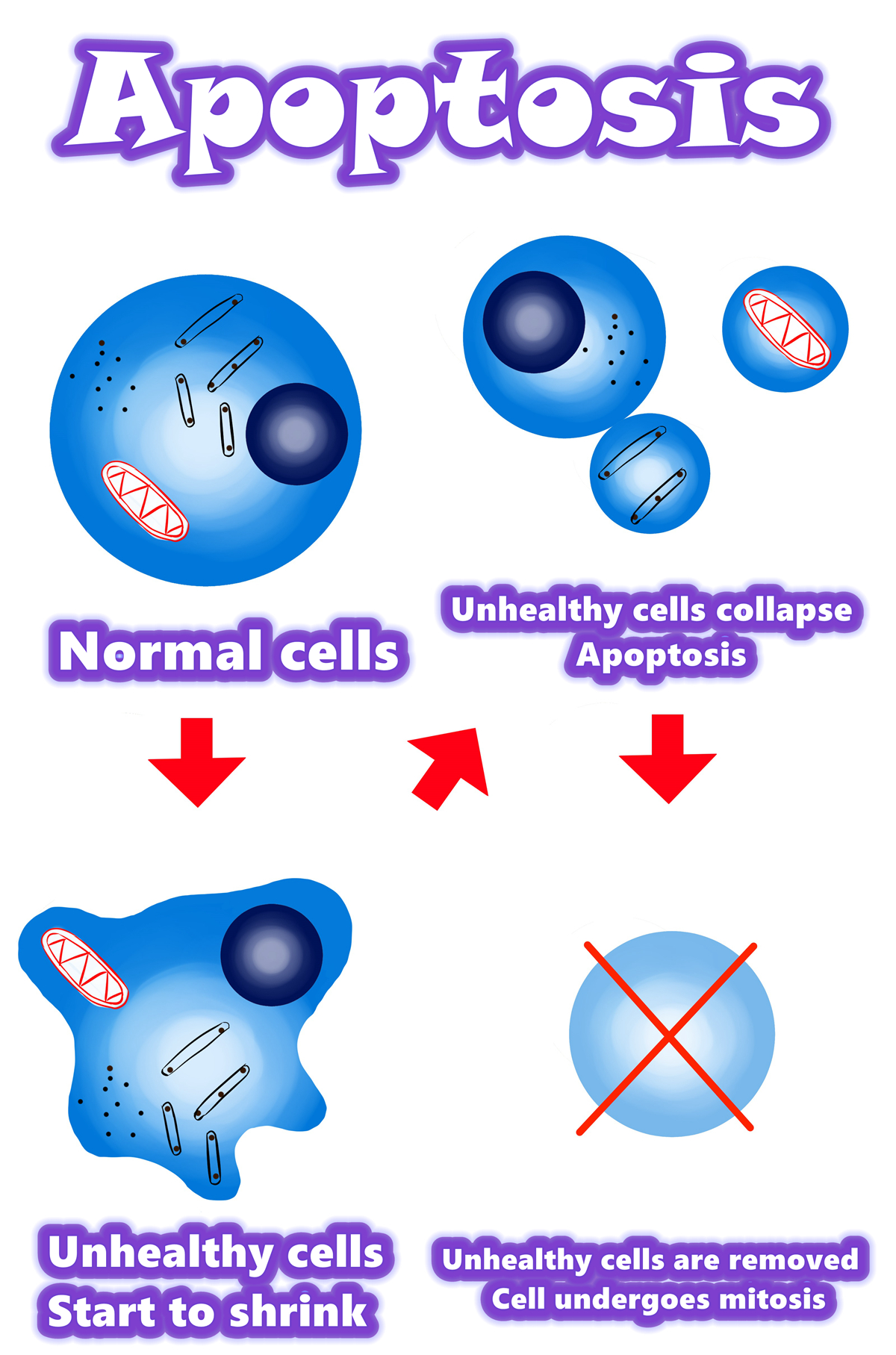
Overview of apoptosis
•Programmed cell death
•Apoptosis is a form of programmed cell death, or “cellular suicide.”
•Apoptosis is different from necrosis, in which cells die due to injury.
•Apoptosis removes cells during development, eliminates potentially cancerous and virus-infected cells, and maintains balance in the body.
Why do cells undergo apoptosis?
- Basically, apoptosis is a general and convenient way to remove cells that should no longer be part of the organism.
- Some cells are abnormal and could hurt the rest of the organism if they survive, such as cells with viral infections or DNA damage.
- Apoptosis is part of development
- In many organisms, programmed cell death is a normal part of development.
The relationship between cancer cells and apoptosis
Apoptosis can eliminate infected or cancerous cells.
When a cell’s DNA is damaged, it will typically detect the damage and try to repair it.
If the damage is beyond repair, the cell will normally send itself into apoptosis, ensuring that it will not pass on its damaged DNA.
When cells have DNA damage but fail to undergo apoptosis, they may be on the road to cancer.
However, “successful” cancer cells successfully evade the process of apoptosis.
This allows them to divide out of control and accumulate mutations (changes in their DNA).
Apoptosis is key to immune function
Apoptosis also plays an essential role in the development and maintenance of a healthy immune system.
Where are the weaknesses and symptoms of cancer cells?
The symptoms of cancer cells are in the nucleus.
The nucleus controls the outer cytoplasm, cell composition, cell viability, etc.
DNA mutations also mutate in the nucleus.
Therefore, to treat cancer cells, we must first enter the nucleus.
Let the “regulatory cell gene” mechanism enter the nucleus to regulate
Are cancer cells aggressive?
After the action of Solamargine, the aggressiveness of cancer cells is alleviated.
So after using Solamargine, many patients feel that I am half better.
Although the tumor does not disappear quickly, patients feel that the degree of aggressiveness is reduced.
Extraordinary Solamargine (Role, Principle, Action, Mechanism, Function, Work).
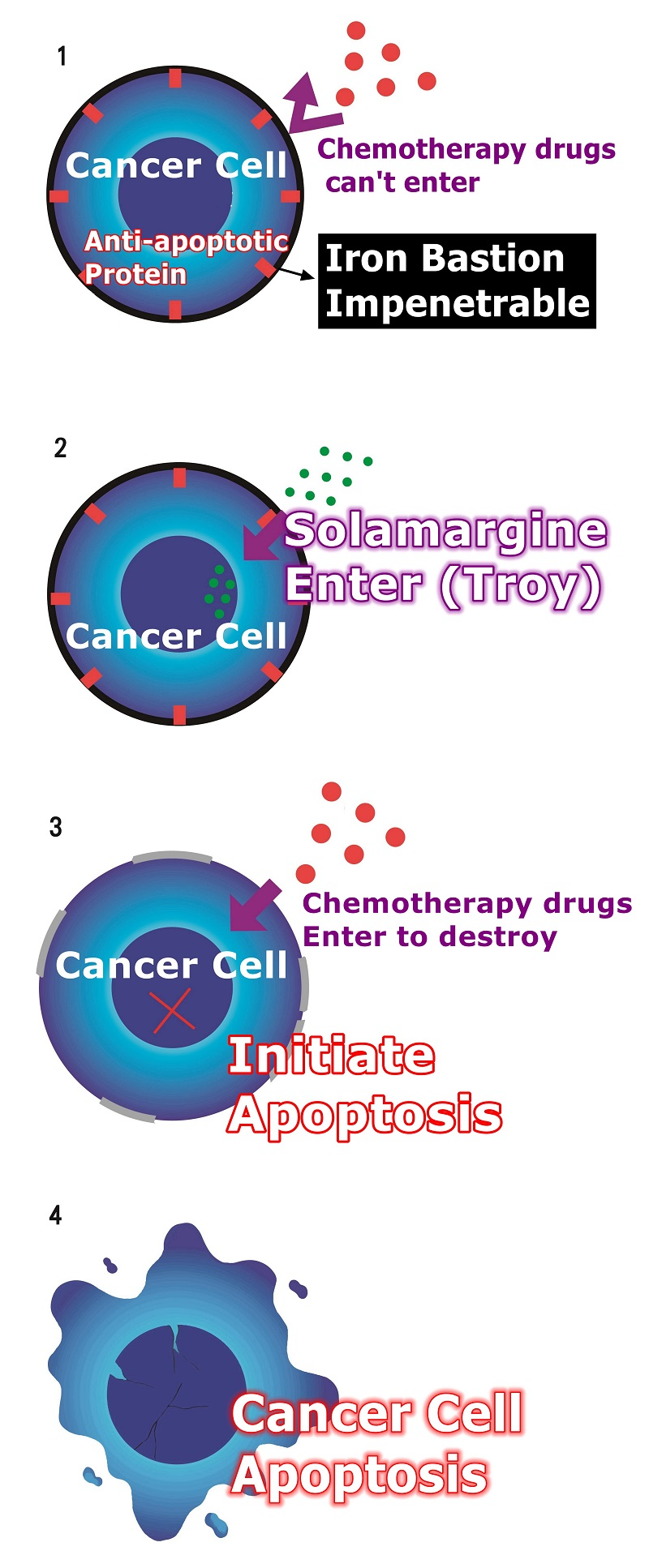
Solamargine's major function mechanism:
When Solamargine enter,
Solamargine activates receptors that are turned off by cancer cells, allowing cancer cells to modulate again.
Solamargine modulates the anti-modulates genes of cancer cells, making cancer cells less resistant.
Reduced drug resistance
When cancer cells are less resistant to drugs, chemotherapy becomes more effective.
Solamargine modulates the mutated genes in cancer cells and then initiates cancer cell apoptosis to achieve anti-cancer effects.
Solamargine combined with which chemotherapy drugs are more effective in treating cancer cells?
Solamargine vs cancer
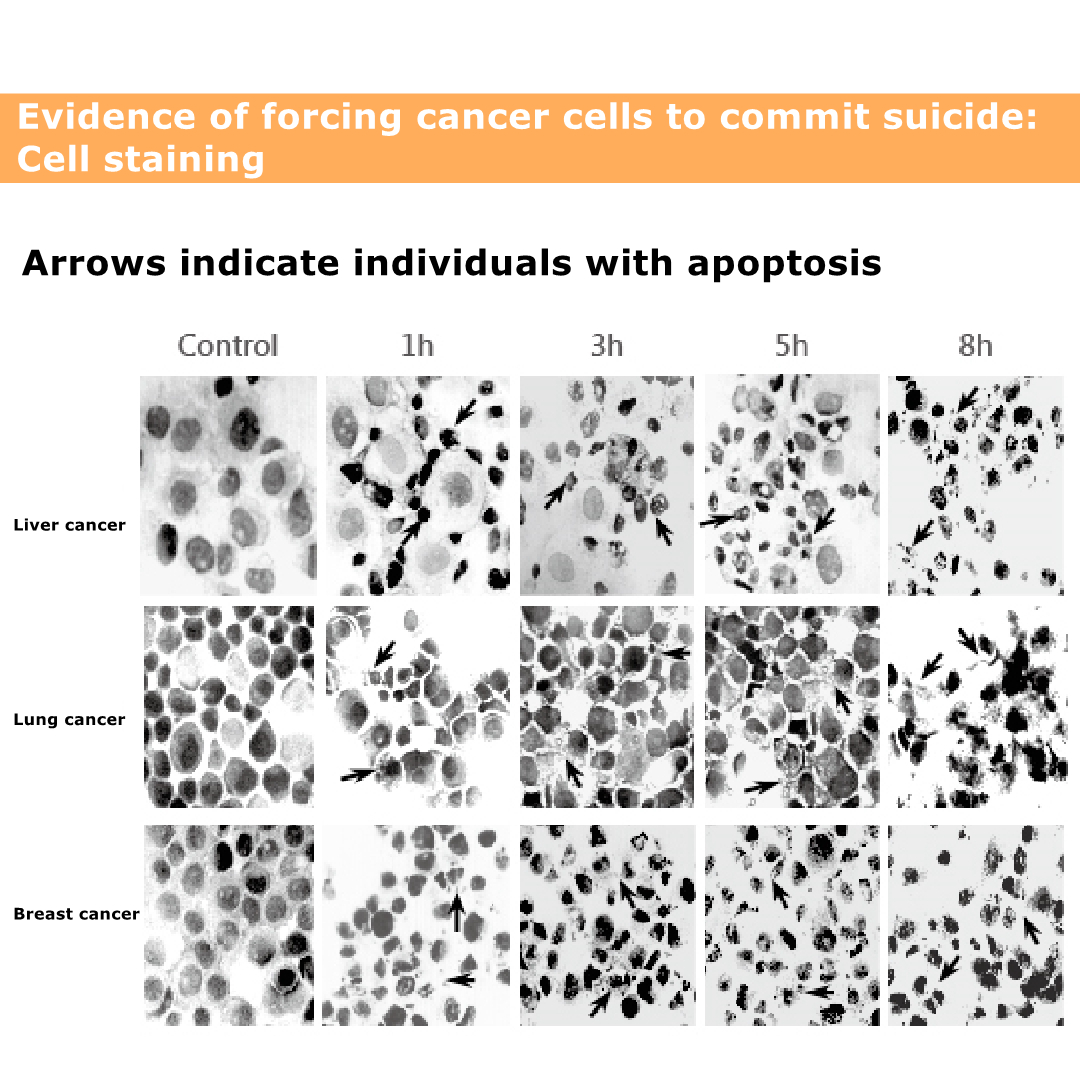
Solamargine vs cancer
The picture shows the death of cancer cells.
The black and black parts are cancer cell nuclei.
Even if the nucleus ruptures, the cancer cells will die.
The figure shows that cancer cells can cause death.
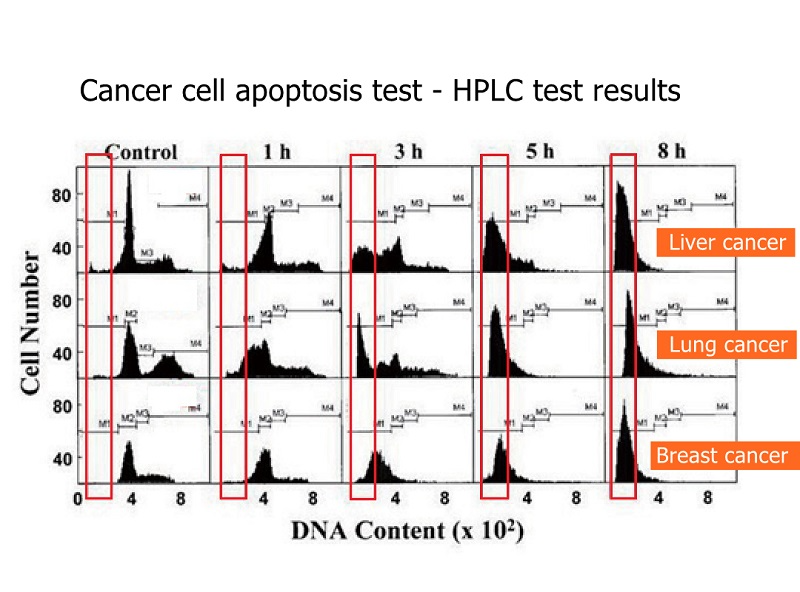
The figure shows that cancer cells can cause death.
The figure shows that the death of lung cancer cells is relatively slow, and it will not be obvious until eight hours later.
The figure shows that the death of liver cancer cells is very obvious, even more obvious in eight hours.
The graph shows that breast cancer cells die faster. It was obvious from the beginning that breast cancer is easy to treat, and patients with breast cancer need not worry.
Best Chemotherapy Adjuvant. (1+1>487%)
Effectively improve chemotherapy effect and treatment.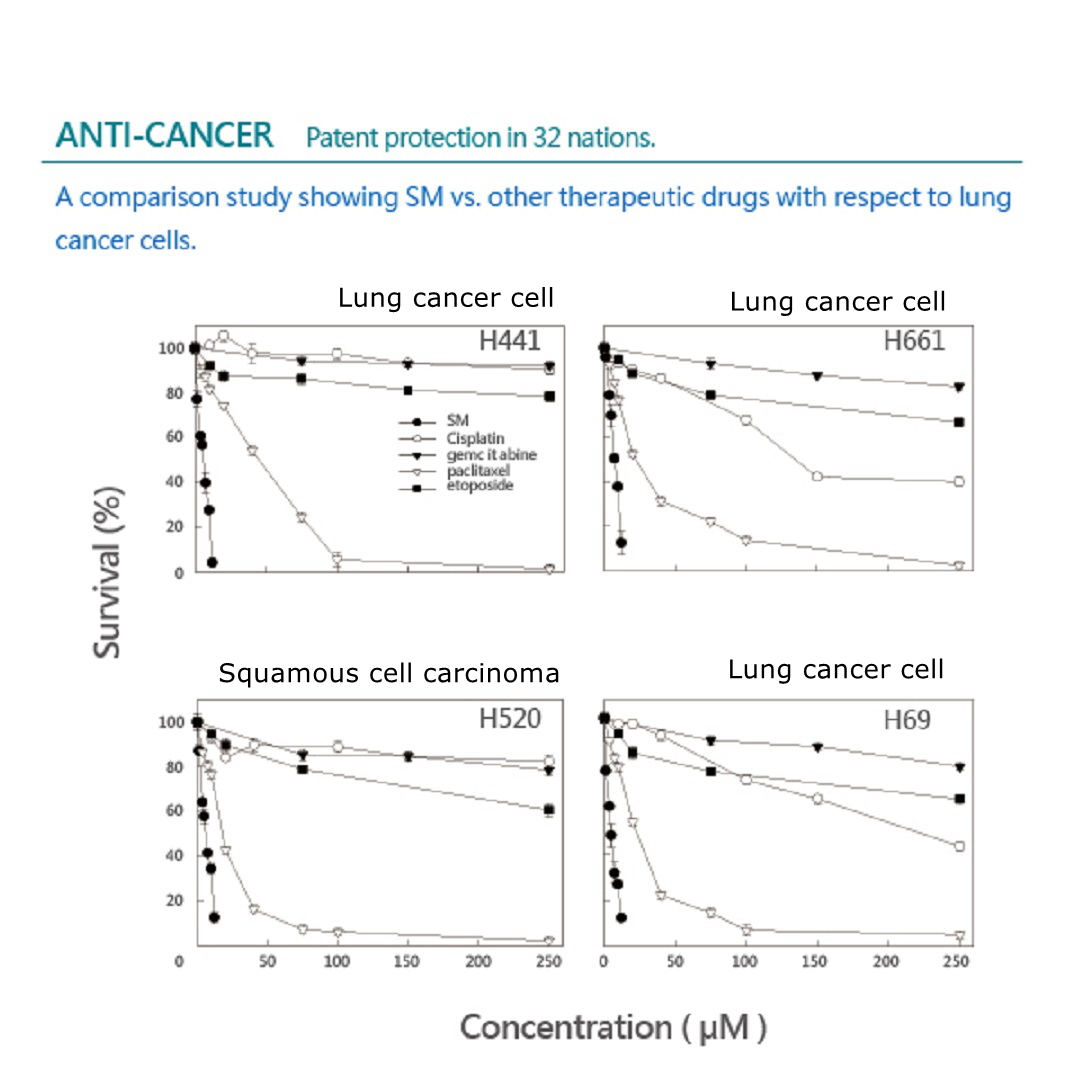
ANTI-CANCER
Patent protection in 32 nations.
A comparison study showing Solamargine vs. other therapeutic drugs with respect to lung cancer cells.
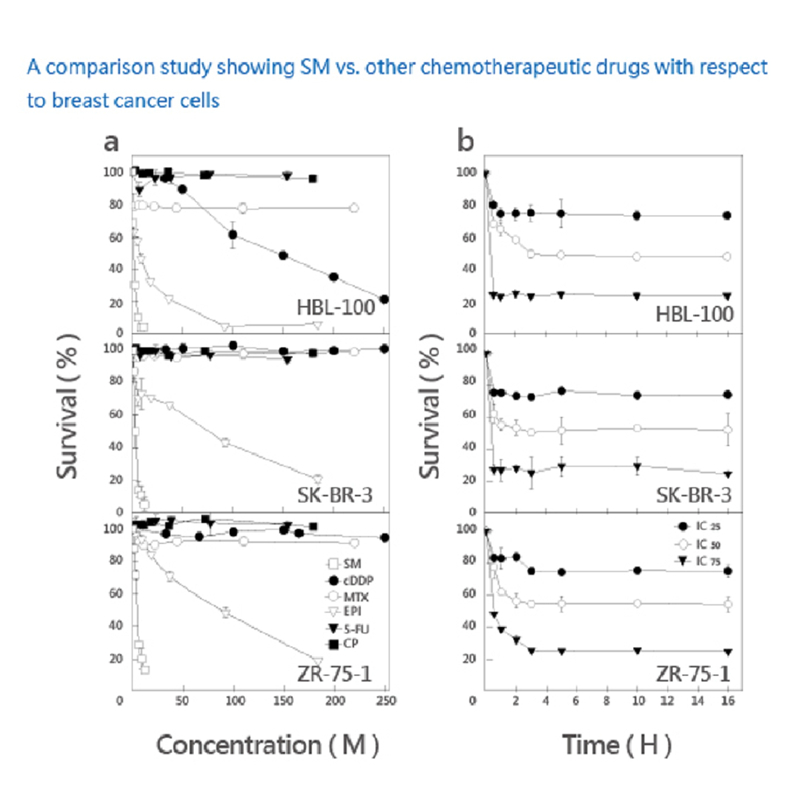 A comparison study showing Solamargine vs. other chemotherapeutic drugs with respect to breast cancer cells.
A comparison study showing Solamargine vs. other chemotherapeutic drugs with respect to breast cancer cells.
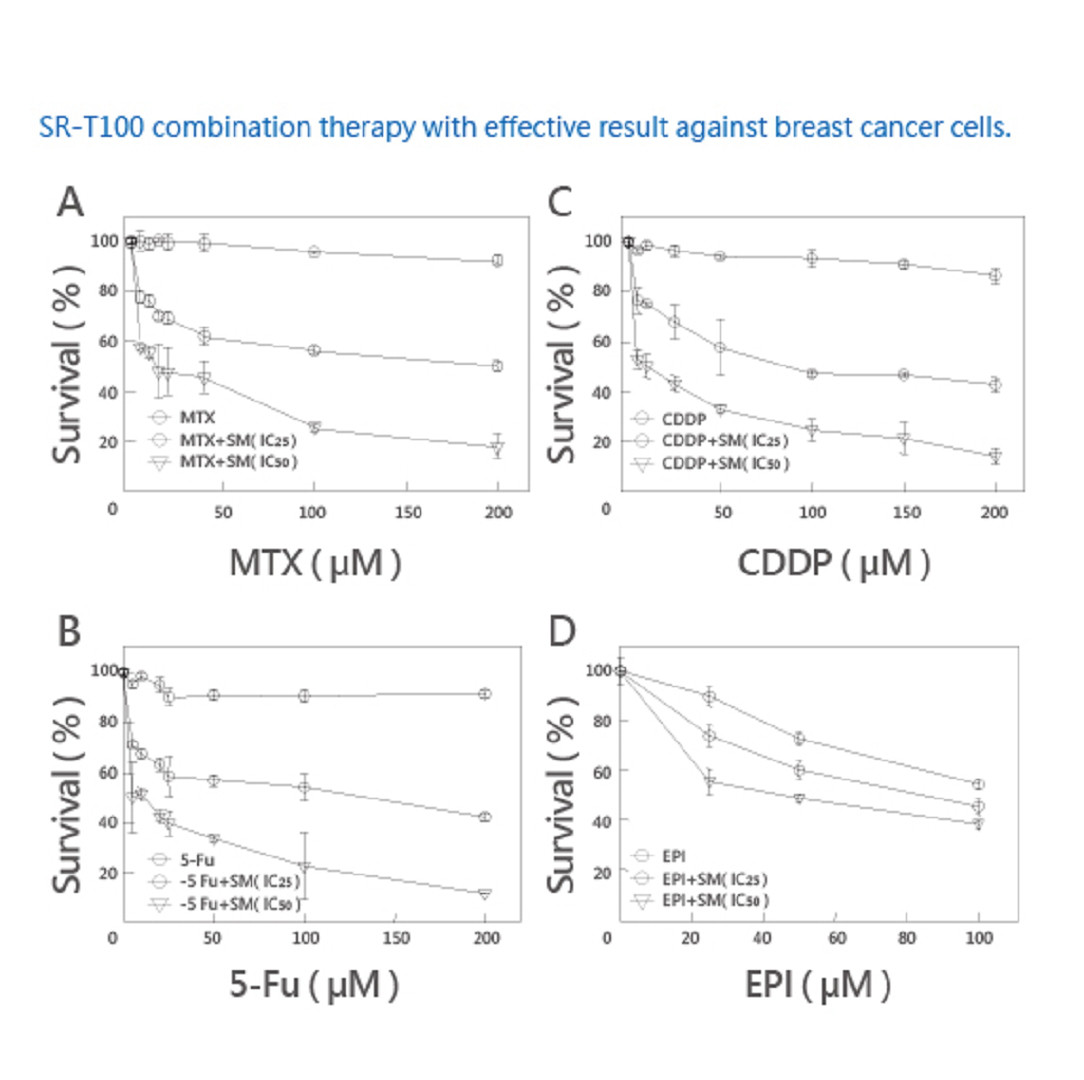
SR-T100 combination therapy with effective result against breast cancer cells.
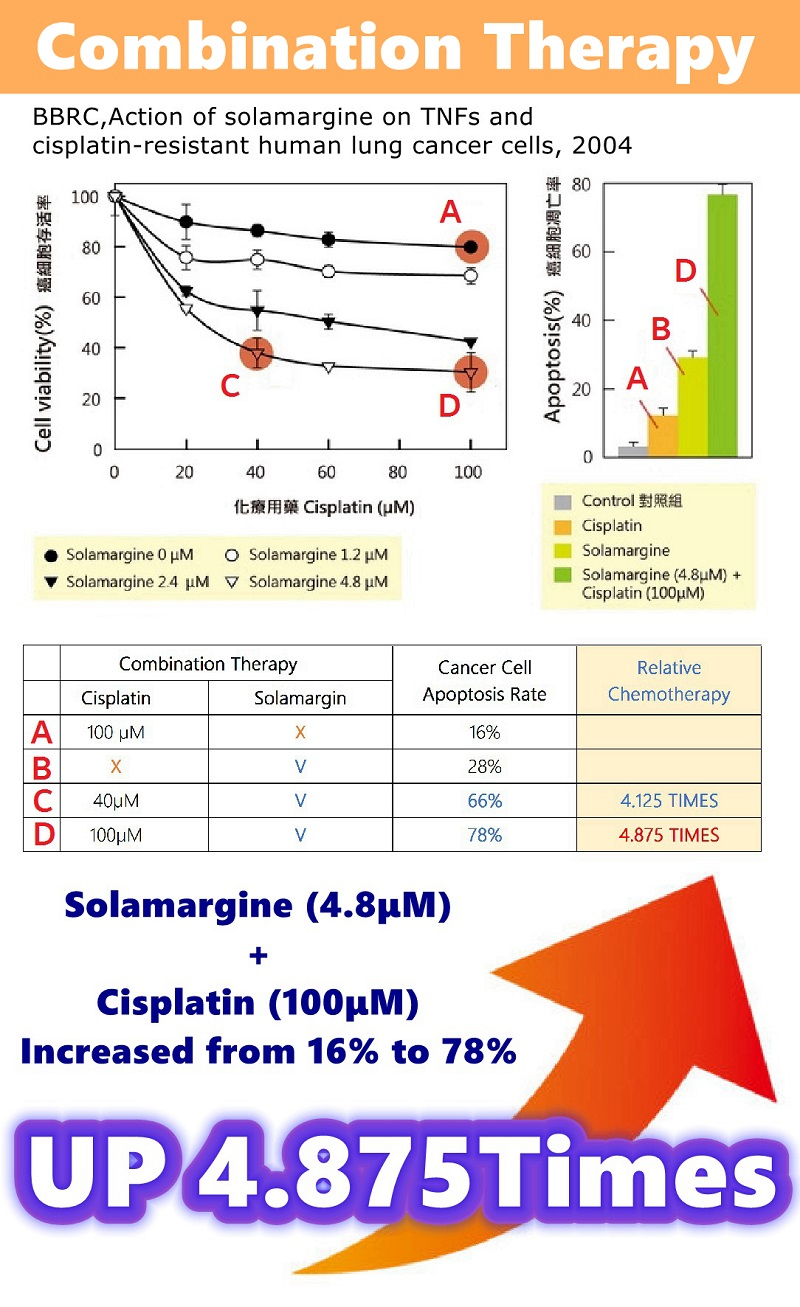
Combination Therapy | Research results for lung cancer cells.
A. Chemotherapy (100μM), 16% of cancer cell apoptosis.
B. Alone SM (4.8μM), 28% of cancer cell apoptosis.
C. SM (4.80μM) + Chemotherapy (40μM), 66% of cancer cells apoptosis.
D. SM (4.80μM) + Chemotherapy (100μM), 78% of cancer cell apoptosis.
SM has a clearing effect better than Chemotherapy.
The combined treatment of Solamargine and Chemotherapy significantly increased the apoptosis of lung cancer cells.
SM (4.8μM) + Chemotherapy (40μM), increased from 16% to 66% (up to 4.125 times).
SM (4.8μM) + Chemotherapy (100μM), increased from 16% to 78% (up to 4.875 times).
Reorganized from: BBRC. Action of Solamargine on TNFs and drug-resistant human lung cancer cells 2004.
The best solution for cancer cells.
